Healthcare Workflow Automation: How to Stop Drowning in Manual Tasks and Reclaim Your Team's Time
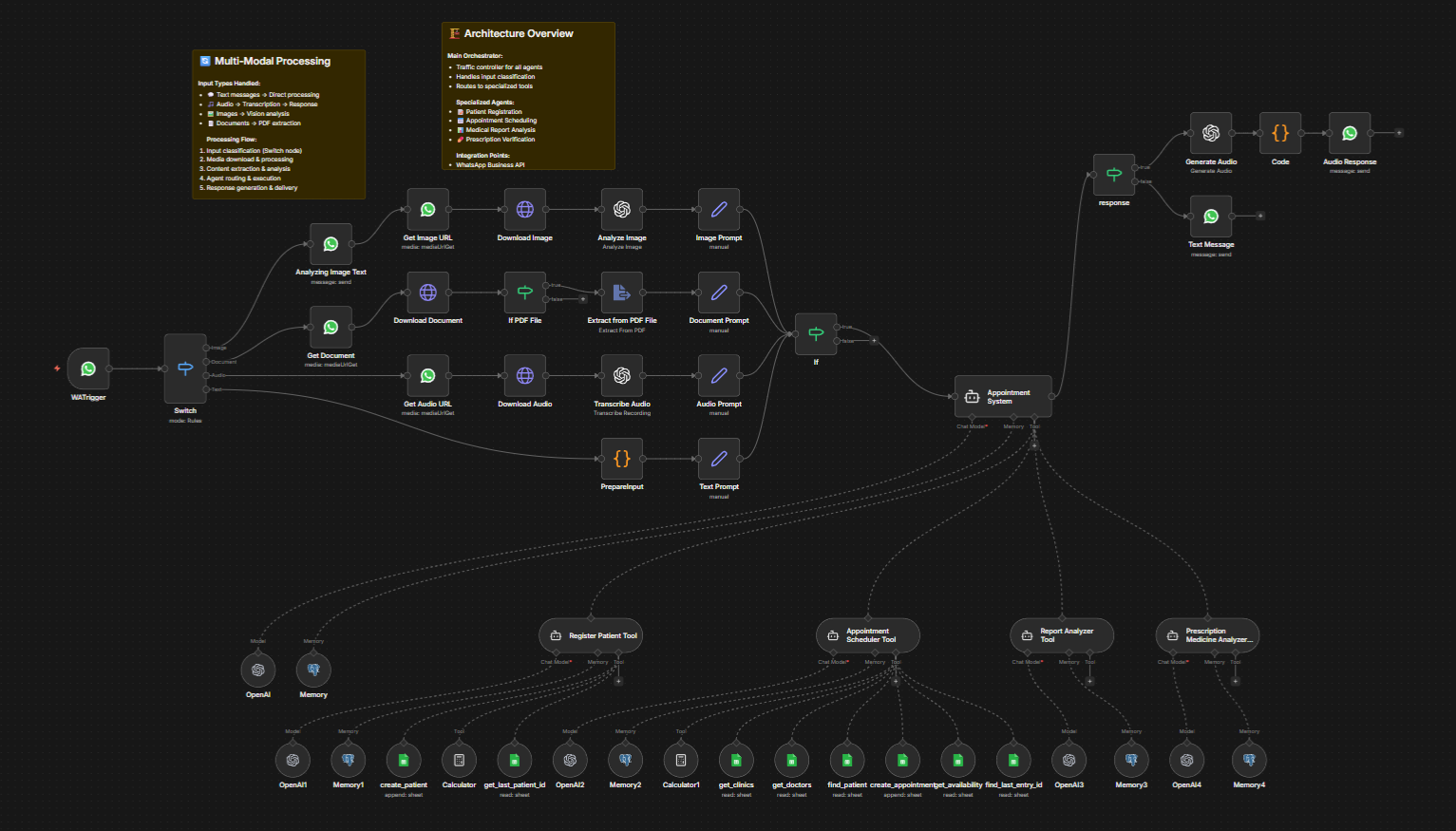
Discover how healthcare workflow automation can eliminate manual prior auth, billing, and referral tasks. Saving time, reducing errors, and improving patient care. If you need help with anything, get in touch with jeroen[at]clsystems[dot]nl as he has deep knowledge of n8n workflows.
Why Healthcare Is Still Drowning in Manual Work, And What to Do About It
If you work in healthcare administration, you already know the feeling: it's 4:30 PM, your inbox has forty unread emails, someone in billing is still on hold with an insurance company, a referral fax came through illegible, and three patients called to ask why their prior authorization hasn't been approved yet. You didn't get into healthcare to spend your days on hold. Neither did your physicians. Yet here you are.
The numbers behind this frustration are staggering. Physicians spend an average of 13 hours per week dealing with prior authorizations alone, nearly a full working day and a half every single week, consumed by a single administrative task. A full 93% of providers say that prior authorization delays directly harm patient care. Meanwhile, manual insurance eligibility verification takes roughly 16 minutes per transaction, and checking on a claim status manually burns about 25 minutes. Multiply those figures across hundreds of patients per month and you're looking at dozens of staff-hours evaporating into administrative overhead every single week.
The frustrating part is that most of this work is repetitive, rule-based, and entirely automatable. It doesn't require clinical judgment. It doesn't require empathy or human connection. It requires checking a box, pulling a number, sending a form, and updating a record, tasks that software can handle faster, more accurately, and without ever needing a coffee break. This guide is for the healthcare administrators, clinic managers, billing coordinators, and practice owners who are exhausted by manual workflows and are ready to understand what modern healthcare workflow automation actually looks like in practice.
The Hidden Cost of Manual Healthcare Workflows
Before diving into solutions, it's worth understanding the full scope of the problem, because most healthcare organizations are only aware of the symptoms, not the systemic cost.
Time Theft Is Everywhere
Consider intake alone. When a new patient calls to schedule an appointment, someone on your team manually enters their demographic information, calls or faxes the insurance company to verify eligibility, enters that data into the EHR, and then repeats variations of this process at every subsequent visit. Sixteen minutes per eligibility verification adds up fast. For a practice seeing 50 new patients per week, that's over 13 hours of staff time spent on one sub-step of one workflow, before a single clinical interaction has happened.
Then there's referral management. A remarkable 56% of providers still send referrals via fax. Fax. In an era of cloud computing and real-time APIs, more than half of the healthcare system is relying on a technology that predates the internet to coordinate care between providers. Faxes get lost. They arrive unreadable. They sit in a queue for hours. They require someone to physically walk to a machine, retrieve the document, manually enter the data into a system, and then call to confirm receipt. Every single step in that chain is a failure point.
Revenue Is Leaking Through Administrative Gaps
Credentialing delays create revenue impacts at 46% of healthcare organizations. When a new provider can't see patients because their credentialing paperwork is still being processed manually, passed between email threads, chased via phone calls, waiting on someone to find the right form, that provider is essentially invisible to payers. Every day of delay is a day of revenue that can never be recovered.
Fifty-two percent of organizations still have entirely manual credentialing workflows. That means more than half of healthcare organizations are managing one of their most compliance-sensitive, revenue-critical processes through spreadsheets, email chains, and file folders. The risk isn't just inefficiency, it's audit exposure, compliance failure, and the kind of credentialing gaps that lead to claim denials down the line.
Clinician Burnout Is Partly an Administrative Problem
Seventy-four percent of clinicians report that documentation time actively impedes their ability to provide patient care. That's not a technology problem or a staffing problem, it's a workflow problem. When physicians are spending a third of their working week on prior authorizations and EHR documentation, the burnout that follows isn't surprising. And only 44% of clinicians are satisfied with how well their EHR systems interoperate with other platforms, meaning even the technology they do have often creates more work rather than less.
The cumulative effect is an administrative burden so heavy that it reshapes the entire character of healthcare work. Staff turnover increases. Errors multiply. Patients wait longer. Revenue cycles extend. And everyone in the building feels like they're running on a treadmill that keeps getting faster.
Six Healthcare Workflows That Are Ready to Be Automated Right Now
The good news is that the most painful administrative workflows in healthcare are also among the most automatable. Here's a concrete look at six areas where workflow automation delivers measurable relief.
1. Patient Intake and Registration
Traditional patient intake is a cascade of redundant manual steps: the patient fills out a paper form (or a PDF that has to be printed, signed, scanned, and emailed back), a staff member re-enters all of that information into the EHR, someone else verifies insurance eligibility by phone or portal, and then the same data gets re-entered into the billing system. Information is typed three or four times, creating multiple opportunities for transcription errors.
A fully automated intake workflow looks completely different. The patient receives a digital intake form via text or email before their appointment. They complete it on their phone. Upon submission, the automation triggers an immediate insurance eligibility check through an API connection to the payer or a clearinghouse like Availity or Change Healthcare. Verified insurance information flows directly into the EHR via an HL7 or FHIR integration. The appointment is confirmed automatically. A demographic record is created. A billing record is initialized. All of this happens without a single staff member touching a keyboard.
The downstream impact is significant: fewer data entry errors, faster check-in times, more accurate billing from the start, and staff freed up to handle the work that actually requires a human being.
2. Prior Authorization and Insurance Verification
Prior authorization is arguably the single most painful administrative workflow in American healthcare. It requires pulling clinical documentation, submitting it to the payer in a specific format, following up, often repeatedly, and then communicating the result back to the care team and the patient. When done manually, it consumes that 13-hour-per-week figure cited earlier.
Automation can't replace every element of PA, some decisions genuinely require clinical review. But it can dramatically compress the surrounding administrative work. An automated PA workflow can monitor for upcoming appointments that require authorization, pull the relevant clinical criteria from the EHR, pre-populate the payer's submission form using integrated data, submit electronically where supported, and then monitor for a response. When a decision comes back, the system updates the EHR automatically and sends a notification to the care team and patient.
Similarly, insurance eligibility verification can be automated to run as a scheduled batch process, checking every patient on tomorrow's schedule against payer APIs the evening before, flagging any eligibility issues for a staff member to review in the morning rather than discovering problems at the front desk while a patient is waiting.
3. Appointment Reminders and No-Show Reduction
No-shows cost the U.S. healthcare system an estimated $150 billion per year. Most no-shows happen not because patients don't want to come, but because they forgot, got confused about the time, or didn't know they needed to reschedule. This is an automation problem with an obvious solution.
An automated reminder workflow can send a confirmation text or email the moment an appointment is scheduled, followed by a reminder 48 hours before and another the morning of. If the patient needs to reschedule, a simple reply or click triggers an automated rescheduling flow that updates the EHR calendar and opens the slot for another patient. If the appointment requires pre-visit preparation, fasting, paperwork, a specific arrival time, those instructions can be included in the reminder automatically, triggered by the appointment type in the EHR.
Practices that implement multi-touch automated reminder systems typically see no-show rates drop by 25–40%. That's not a marginal improvement, it's a fundamental change to the economics of a practice.
4. Referral Management and Fax-to-Digital Workflows
Given that 56% of referrals still travel by fax, one of the highest-ROI automations in healthcare is the conversion of incoming faxes into structured digital workflows. This sounds complicated, but it's increasingly accessible thanks to modern OCR (optical character recognition) tools and API-based fax services like Sfax or eFax Corporate that can receive faxes and convert them to digital documents automatically.
Here's how an automated referral workflow might function: An incoming fax is received digitally and immediately routed to an OCR process that extracts key data, referring provider, patient name, date of birth, diagnosis code, requested service. That data is validated against the EHR to check for an existing patient record. If the patient exists, the referral data is written into their chart automatically and a task is created for the referral coordinator. If the patient is new, an intake workflow is triggered. A confirmation is sent back to the referring provider automatically.
This turns a process that previously involved printing, reading, manually entering data, filing paper, and making confirmation phone calls into a process that takes seconds and creates a clean digital audit trail.
5. Billing, Claims, and Denial Management
Medical billing is one of the most complex and error-prone administrative domains in any industry. Claim denials cost the average hospital $5 million per year, and a significant portion of those denials are caused by preventable administrative errors, wrong modifier, missing prior auth number, incorrect patient data, that automation can catch before submission.
An automated billing workflow can include pre-submission validation rules that flag common denial triggers before a claim ever leaves the practice. When a denial does arrive, an automation can parse the denial reason code, identify the appropriate corrective action (resubmit with additional documentation, appeal with clinical notes, correct a coding error), and route the case to the right staff member with all the context they need already assembled. High-volume, low-complexity denials, like timely filing errors or eligibility issues, can often be resolved and resubmitted automatically without human intervention.
Claim status checks, which consume roughly 25 minutes each when done manually, can be automated to run on a schedule, pulling updates from payer portals or clearinghouses and updating the practice management system automatically. Staff can shift their attention from checking claim status to actually resolving the cases that need resolution.
6. Provider Credentialing and Staff Onboarding
Credentialing is simultaneously one of the most compliance-critical and most poorly automated workflows in healthcare. With 52% of organizations still managing it entirely manually, the exposure is substantial. Credentialing involves tracking expiration dates for dozens of documents per provider, licenses, DEA certificates, malpractice insurance, board certifications, and ensuring that re-credentialing applications are submitted to every relevant payer on time.
An automated credentialing workflow can maintain a centralized database of all provider credentials with automated expiration tracking. When a document is approaching expiration, say, 90 days out, the system automatically sends a reminder to the provider and their administrative contact, creates a task in the workflow system, and begins populating the renewal application with information already on file. When new credentials are received, they can be distributed automatically to all payers where the provider is credentialed.
For new provider onboarding, the entire credentialing packet, including CAQH enrollment, primary source verification requests, and payer-specific applications, can be initiated from a single trigger when a new hire record is created in the HR system. This turns a process that often takes 60–120 days when managed manually into one with clear accountability, automated follow-through, and no dropped balls.
What Is n8n, And Why Is It Especially Suited for Healthcare Automation?
At this point, you might be thinking: "This all sounds great, but we're a mid-sized medical group, not a tech company. We don't have an engineering team to build custom integrations."
This is exactly where n8n comes in.
n8n (pronounced "n-eight-n") is an open-source workflow automation platform that allows you to connect virtually any application, database, or API, without writing complex code for every connection. Think of it as the connective tissue between all the systems your organization already uses: your EHR, your practice management system, your clearinghouse, your payer portals, your scheduling tool, your HR platform, your fax service, your communication tools.
n8n uses a visual, node-based interface where workflows are built by connecting triggers and actions. A trigger might be "a new patient form is submitted" or "it's 6 PM the day before tomorrow's schedule" or "a claim denial code is received from the clearinghouse." An action might be "write this data to the EHR," "send this text message," "create this task in our workflow system," or "check eligibility via the Availity API."
What makes n8n different from other automation tools in a healthcare context is its flexibility and its deployment model. Because n8n is open-source and can be self-hosted, it can be deployed inside your own infrastructure, which matters enormously for HIPAA compliance. You're not sending protected health information to a third-party cloud service you don't control; you're running automation inside your own environment, on your own servers, with your own security controls. For cloud deployments, n8n also offers enterprise-grade infrastructure with appropriate compliance controls.
n8n has native integrations with hundreds of applications, including tools like Google Workspace, Microsoft 365, Slack, Jira, and databases like PostgreSQL and MySQL, and its HTTP Request node means it can connect to virtually any system with an API, including most modern EHRs and clearinghouses. Custom webhooks allow it to receive data from systems that push rather than pull.
For healthcare organizations, n8n can be the automation layer that sits between your existing systems and makes them work together the way they were always supposed to. You don't need to replace your EHR. You don't need to buy an expensive point solution for every workflow problem. You need a platform that can read from your EHR, call a payer API, update a spreadsheet, send a text message, create a task, and log everything, and do it reliably, at scale, on a schedule or in real time.
And because n8n is designed to be used by teams with varying levels of technical sophistication, from IT administrators who want to write custom code nodes to operations managers who want to configure a visual workflow, it bridges the gap between the clinical/administrative world and the technical world in a way that most automation platforms don't.
Getting Started: A Practical Path Forward
Healthcare automation doesn't have to be an all-or-nothing transformation. The most effective approach is to start with the workflow that is causing the most pain right now, the one where staff are loudest in their frustration, where errors are most frequent, or where the revenue impact is most visible.
For most practices, that starting point is either prior authorization or eligibility verification, simply because those workflows consume so much staff time and have such a direct impact on patient care and revenue. Others find that appointment reminders offer the fastest path to ROI because the technology is straightforward and the results are measurable within weeks.
The key questions to answer before starting any automation initiative:
1. What data needs to move, and between which systems? Map out the inputs and outputs of the workflow you want to automate. Where does the data come from? Where does it need to go? What transformation or decision logic happens in between?
2. Which of your existing systems have APIs? Most modern EHRs, Epic, Cerner, Athenahealth, Kareo, eClinicalWorks, have API access of some kind, though the depth of access varies. Your clearinghouse almost certainly does. Your scheduling tool probably does. Start with the systems that are easiest to connect.
3. What are your compliance requirements? HIPAA compliance shapes every technical decision. Any automation platform handling PHI must be evaluated for its data handling practices, encryption standards, access controls, and BAA (Business Associate Agreement) availability. n8n's self-hosted option sidesteps many of these concerns by keeping data within your own infrastructure.
4. Who will own and maintain the workflows? Automation is not a set-it-and-forget-it solution. Payer requirements change. EHR fields change. Workflow steps evolve. Someone on your team needs to own the automation layer and be empowered to update it as your needs change.
If you're ready to move from manual chaos to automated clarity, the place to start is a clear-eyed audit of your most time-consuming workflows, and a conversation about which of them are actually rule-based enough to automate. The answer, in most healthcare organizations, is: most of them.
The Bottom Line
Healthcare administration is hard enough without doing manually what software can do automatically. The statistics are clear: prior authorizations are stealing physicians' time and delaying care, manual eligibility verification is consuming staff hours that should be spent on patients, fax-based referrals are creating errors and delays, and credentialing workflows are causing real revenue loss at nearly half of all healthcare organizations.
Workflow automation is not a futuristic concept. It is available today, it is accessible to organizations without large IT teams, and it does not require replacing the systems you've already invested in. Platforms like n8n make it possible to connect your existing tools, your EHR, your clearinghouse, your scheduling system, your communication tools, into automated workflows that run reliably, consistently, and without manual intervention.
The healthcare organizations that will thrive in the next decade are not the ones with the most staff doing the most manual work, they're the ones that have automated the automatable so that their people can focus on the irreplaceable: patient care, complex clinical decisions, and the human relationships that no workflow can replicate.
If you're ready to explore what healthcare workflow automation could look like for your organization, register for free to learn how to get started with n8n in a healthcare context. Whether you're a solo practice manager or an administrator overseeing a multi-site group, there's a path from where you are today to a significantly less manual tomorrow.
If you need help with anything, get in touch with jeroen[at]clsystems[dot]nl as he has deep knowledge of n8n workflows.
This post is part of an ongoing series on workflow automation for healthcare organizations. Topics include EHR integrations, HIPAA-compliant automation architecture, and department-specific automation guides for billing, credentialing, and clinical operations.


